Ps Ot Normal for Babies to Lose Weight Right After Birth
- Research
- Open up Access
- Published:
Determinants of excessive weight loss in breastfed full-term newborns at a baby-friendly hospital: a retrospective cohort report
International Breastfeeding Journal volume 15, Article number:nineteen (2020) Cite this article
Abstract
Background
Excessive weight loss in newborns is associated with neonatal complications such every bit jaundice and dehydration, which cause renal failure, thrombosis, hypovolemic shock, and seizures. The identification of the take a chance factors for excessive weight loss will help to discover preventive measures. The aim of this study was to decide the factors associated with excessive weight loss, divers as weight loss of ≥10%, in breastfed full-term newborns in Nihon.
Methods
The present retrospective study, which was performed in a tertiary perinatal centre accredited as a Baby-Friendly Hospital, included neonates who were born alive with a gestational historic period of ≥37 weeks. Cases of multiple births, admission to the neonatal intensive care unit of measurement (NICU), referral to another facility, or sectional formula feeding were excluded. Multivariate logistic regression analyses were performed to assess the association betwixt maternal or neonatal characteristics and excessive weight loss.
Results
We studied 399 newborns, of whom 164 (41%) had excessive weight loss. According to the adjusted multiple regression analysis, the factors associated with excessive weight loss were an older maternal age, primiparity, and antepartum Caesarean section, with adjusted odds ratios (95% Confidence Intervals [CIs]) of ane.07 (i.02, 1.11), ii.72 (1.69, 4.38), and 2.00 (1.09, 3.65), respectively.
Conclusions
Close monitoring of infants born to older mothers, primiparous mothers, or infants delivered by antepartum Cesarean section is recommended, and earlier supplementation with artificial milk may be considered.
Background
Almost all newborns lose weight in the first days of life [one, 2], and this is chosen physiological weight loss [3]. It is mainly due to fluid reduction [4]. Belatedly cord clamping is related to a higher nativity weight, which results in a greater weight change [5]. Neonatal weight loss is likewise a consequence of the use of adipose tissue as a source of free energy past the newborns [3]. Excessive weight loss is associated with complications such every bit jaundice [6,seven,eight,ix], hypoglycemia [10], and dehydration, which cause renal failure, thrombosis, hypovolemic shock, and seizures [11,12,13,14,fifteen,sixteen,17,18,xix].
Breastfeeding undoubtedly provides health advantages to both the babe and the mother. Supplementation with formula should be avoided unless medically indicated every bit information technology may discourage the initiation and decrease the duration of breastfeeding [20,21,22]. The extent of a newborn's weight loss in the first days of life is used equally an indicator of breastfeeding adequacy [23]. The percent of weight reduction that indicates formula supplementation is controversial [24]. A weight reduction of 10% is frequently practical because it is related to hypernatremic dehydration [25,26,27]. Information technology is important to make up one's mind the hazard factors for excessive weight loss to discover preventive measures.
Caesarean section is a known risk cistron for excessive weight loss among newborns [ane, 28]. All the same, little is known nigh the differences in risk according to the blazon of Caesarean section (antepartum or intrapartum) and the existence of other run a risk factors, especially in newborns at an accredited Baby-Friendly Hospital. The hazard factors identified in the literature differ, depending on the setting [28,29,30,31,32,33]. Therefore, the aim of this study was to determine the factors associated with excessive weight loss in breastfed full-term newborns at a Baby-Friendly Infirmary.
Methods
Study pattern, population, and setting
This was a retrospective observational study with no patient contact. It was conducted at a tertiary perinatal eye (The National Hospital Organization Nagasaki Medical Center) in Nippon. We included live babies who were built-in at ≥37 weeks of gestation between Jan i, 2018, and Dec 31, 2018. We excluded cases of multiple births, cases in which babies were admitted to the neonatal intensive intendance unit (NICU) or referred to other facilities, and cases of sectional formula feeding.
Our hospital is accredited as a Baby-Friendly Infirmary and promotes the initiation of exclusive breastfeeding [34]. A full of 66 facilities, including 27 perinatal centers, are accredited as Infant-Friendly Hospitals in Japan [35]. In our hospital, early cord clamping is performed later a infant is delivered. In add-on, we adhere closely to the "10 Steps to Successful Breastfeeding" [34]. We do not have whatever lactation consultants. However, trained midwives or nurses help mothers afterwards delivery to assure adequate breastfeeding. Temporary formula feeding is considered in cases of weight loss ≥x% in relation to the birth weight after a concrete examination and blood tests, including the blood levels of glucose, urea nitrogen, and electrolytes, are performed. However, in cases of medical needs such as constant hypoglycemia or dehydration, minimal h2o or formula is given to infants even earlier weight loss reaches 10%. Hospital discharge at our facility routinely occurs when the infants are 5 days one-time in the case of vaginal delivery or 6 days old afterward a Caesarean department. All newborns are weighed daily between nascency and belch while naked with an electronic calibration by a nurse or a midwife. Discharge is postponed if there are whatever maternal or neonatal complications, and discharge is non permitted until the infant'south weight begins to increase after its nadir.
Data collection and definitions
We retrospectively obtained the demographic and perinatal data from the patients' medical records. The following maternal and neonatal variables were assessed: maternal historic period, prepregnancy weight, prepregnancy torso mass index (BMI), parity, infertility treatment, maternal weight gain during pregnancy, hypertension, diabetes, gestational week at delivery, use of magnesium sulfate in labor, use of oxytocin in labor, mode of delivery (vaginal delivery, intrapartum Caesarean department, or antepartum Caesarean section), postpartum hemorrhaging, maternal hemoglobin subsequently delivery, nascency weight, newborn sex, apply of infant formula or water before a weight loss of ≥10% and neonatal jaundice requiring phototherapy. Prepregnancy BMI was calculated with maternal elevation at the first antenatal visit and self-reported prepregnancy weight. Maternal hypertension was defined equally a systolic blood pressure level ≥ 140 mmHg or a diastolic blood pressure ≥ 90 mmHg, regardless of the fourth dimension of diagnosis, including before pregnancy, in pregnancy, and during the hospital stay. It included chronic hypertension, gestational hypertension, preeclampsia, and eclampsia. Diabetes included type ane, blazon 2, and gestational diabetes. Operative deliveries were classified every bit 'antepartum' if they were performed before the onset of labor and 'intrapartum' if they were performed after labor began [36]. The offset of labor was defined as regular contractions occurring < 10 min apart and progressive cervical dilation or effacement [37]. All elective Caesarean sections were categorized equally antepartum Caesarean sections. Emergency Caesarean sections could be antepartum or intrapartum Caesarean sections. Postpartum hemorrhaging was divers as a cumulative blood loss of ≥1000 mL inside 24 h of the nativity procedure, regardless of the mode of delivery [38]. Hemoglobin levels were measured inside ii–three days after delivery.
Outcomes
The upshot was excessive weight loss, which was defined every bit a weight reduction of ≥x% in the offset 5 days of life in relation to the nascency weight.
Secondary analysis
We examined whether there were any newborns who required intravenous therapy due to hypoglycemia or dehydration. We also investigated the association between neonatal jaundice requiring phototherapy and a higher weight loss.
We analyzed the claret test results of newborns who experienced a weight reduction of ≥10%. The plasma osmolality was calculated by the following formula: plasma osmolality = (sodium [mEq/L] × 2) + (glucose [mg/dL] / 18) + (claret urea nitrogen [mg/dL] / 2.8). The mean plasma osmolality results were compared amongst the groups stratified co-ordinate to the way of delivery.
Statistical analysis
Information were entered in the Microsoft Excel software program (version fourteen.1.0; Microsoft®, Redmond, WA, U.s.) and exported to EZR (version 3.1.2; Saitama Medical Middle, Jichi Medical University, Saitama, Nihon), which was used to carry out the statistical analyses. Descriptive statistics were performed to determine the means (± standard deviations) and percentages. The Kolmogorov–Smirnov test was used to examine normality. The Pupil's t-test or the Isle of mann–Whitney U examination was used to clarify 2 continuous variables, as advisable. The ANOVA examination or the Kruskal-Wallis exam was used to analyze 3 continuous variables, as appropriate. Pearson'southward chi-squared test was used to analyze chiselled variables. Univariate logistic regression analysis of these variables was performed to estimate the rough odds ratios and their 95% conviction intervals (CIs). Then, we conducted multivariate logistic regression analysis. Factors with p values < 0.05 according to the univariate analysis were entered into the multivariate analysis. Neonatal jaundice requiring phototherapy was not included in the regression model of the primary outcome because neonatal jaundice is not the cause but the result of weight loss. Statistical interaction was examined between parity and the mode of commitment. P values < 0.05 were considered to indicate statistical significance.
Ethical considerations
This study was approved past the Research Ethics Commission of the National Infirmary Organization Nagasaki Medical under protocol number 2019079, approved on October 10, 2019, with opt-out consent to obtain patient information from the medical records. No ethical problems arose during this report as it was retrospective and all data were bearding.
Results
A total of 452 babies were born live with a gestational age of ≥37 weeks during the study period, and 399 newborns were included in the current study after excluding 53 cases: 26 for multiple births, 22 for access to the NICU, 2 for referral to another facility, and 3 for sectional formula feeding. The mean percent of weight reduction was 9.4%. Of these, 164 newborns (41%) lost ≥10% of their body weight (Fig. i). The weight reached its nadir at day 3.0 ± 0.eight (mean ± standard difference).
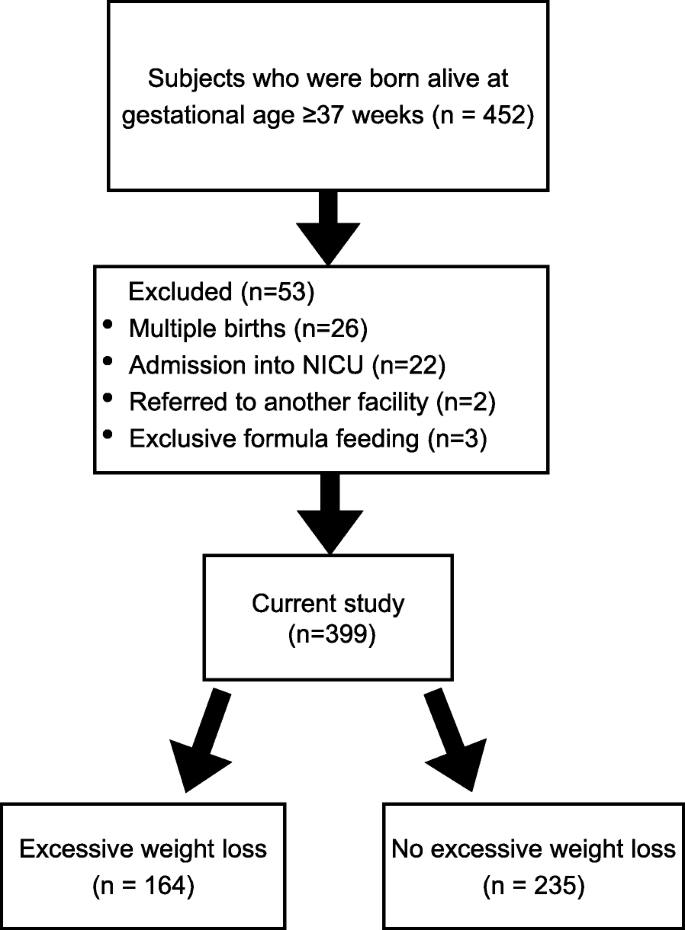
Flow nautical chart of the patients included in this study
Table 1 shows the comparing of the maternal and neonatal characteristics between newborns with and without excessive weight loss. The mothers of newborns with excessive weight loss were older (p = 0.004), had a higher BMI (p = 0.043), were more ofttimes primiparous (p = 0.001), had more frequently received infertility treatment (p = 0.009), had more frequent postpartum hemorrhaging ≥thousand mL (p = 0.013), and had a lower hemoglobin level after delivery (p = 0.013) than mothers of newborns without excessive weight loss (Table 1).
Table ii shows the univariate and multivariate logistic analysis results of the associations between the variables and excessive weight loss in newborns. According to the univariate assay, maternal historic period, primiparity, infertility treatment, antepartum Caesarean section, postpartum hemorrhaging, and the hemoglobin level later on delivery were associated with excessive weight loss in newborns. Meanwhile, according to the adjusted multiple regression analysis, the factors associated with excessive weight loss in newborns were an older maternal age, primiparity, and antepartum Caesarean department, with adjusted odds ratios (95% Confidence Intervals [CIs]) of 1.07 (one.02, one.11), 2.72 (1.69, 4.38), and 2.00 (1.09, 3.65), respectively (Table 2). No statistical interaction was noted between parity and the way of delivery, or betwixt maternal age and infertility treatment.
No total-term newborn included in this study required intravenous therapy due to hypoglycemia or dehydration. Nevertheless, neonatal jaundice requiring phototherapy was associated with a higher weight loss (percentage) (odds ratio: ane.22; 95% CI: 1.05–1.42).
Table 3 shows the laboratory examination results of the newborns who were examined on the day of weight loss ≥x%. The hateful plasma osmolalities on the mean solar day of weight loss ≥ten% were 306, 304, and 303 mOsm/kgH2O in newborns delivered by vaginal delivery, intrapartum Caesarean section, and antepartum Caesarean section, respectively (p = 0.043).
Give-and-take
Our data showed a high hateful per centum of weight reduction (nine.four%) and a high rate (41%) of excessive weight loss in healthy full-term newborns at our heart. The mean percent of weight reduction in our middle was much higher than that reported in the literature in other developed countries (two.four–8.6%) [25,26,27, 31, 39, 40]. This discrepancy may exist partly due to the delayed lactogenesis in Asians compared to other indigenous groups [41]. It is also because we check the weight every day and keep a baby in the hospital until we ostend a nadir of the weight. The charge per unit is also college than that of other perinatal centers accredited as Baby-Friendly Hospitals in Nippon. In 2018, the mean weight reduction rates at 27 perinatal centers accredited as Baby-Friendly Hospitals in Japan were eight.two and eight.nine% for vaginal commitment and Caesarean department, respectively [42]. In comparison, the rates were 9.0 and 9.9% at our eye, respectively [42]. Our cohort's baseline characteristics were similar to those of 27 perinatal centers accredited equally Baby-Friendly Hospitals in Nippon [42]. This divergence of the weight reduction is perhaps related to the loftier rate of exclusively breastfed newborns. The same report showed that the mean rate of exclusively breastfed newborns at infirmary discharge at 27 perinatal centers was 77% [42], while the rate at our center was 84% [42].
An older maternal historic period [29] and primiparity [xix, 30] also have been shown equally risk factors for excessive newborn weight loss in previous studies [29, thirty]. An older maternal age [43, 44] and primiparity [30, 45, 46] are associated with excessive weight loss in newborns due to the delayed onset of lactation.
The most notable finding of this written report was that there was a significant difference in the frequency of excessive weight loss between the newborns delivered past antepartum Caesarean section and those delivered by vaginal delivery, while no marked difference was noted between infants delivered via intrapartum Caesarean section and those delivered by vaginal delivery. Most of the previous studies on this topic did not distinguish between antepartum Caesarean section and intrapartum Caesarean section. Our finding is consistent with one previous study [47]. In addition, an observational cohort written report has demonstrated that main antepartum Caesarean department is an contained gamble factor for the failure of sectional breastfeeding [48]. However, their written report outcome was different from ours, and the study did not distinguish between the experience of never trying to breastfeed and that of trying but not succeeding.
Three hypotheses may explain these findings. First, labor causes hormonal changes in the mother, and these changes promote lactogenesis. Some studies suggest that labor tin can drag the plasma concentrations of oxytocin and prolactin [49, fifty]. Second, labor causes hormonal changes in newborns, and these changes bear on the kidney part and insensible h2o loss. For case, glucocorticoids are known to reduce the rate of insensible water loss in newborns [51], and oxytocin is an antidiuretic [52]. Third, labor itself or the excessive administration of fluids to the mother before she gives birth may affect the amount of total body h2o in the newborn at birth. An observational cohort study has shown that the timing and the amount of maternal intravenous fluids are related to the neonatal output and newborn weight loss [53]. The differences of hateful plasma osmolality on the twenty-four hour period of ≥10% in newborns delivered by vaginal delivery, intrapartum Caesarean section, and antepartum Caesarean department indicated that the newborns delivered past antepartum Caesarean section tended to be born with more body water, and the shedding of this backlog water after birth accounts for function of the weight loss. Further research is necessary to determine the mechanisms involved.
The results of the present study suggest that earlier intervention including closer monitoring of mothers and babies as well as earlier initiation of formula feeding in cases with an older maternal historic period, primiparity, and antepartum Caesarean department may aid to prevent complications in newborns due to excessive weight loss.
Several limitations associated with the nowadays written report warrant mention. Showtime, considering our report population was derived from i hospital in Japan, the generalizability of our report results might be limited to some extent. Second, in that location might be other factors associated with excessive weight loss in newborns. For example, we did not examine the rate of weight loss or the feeding methods in previous pregnancies. In addition, we did not clarify drug apply in labor or pregnancy except for oxytocin and magnesium sulfate use in labor, which might affect babe feeding. 3rd, prepregnancy BMI is subject to retention bias and the timing of weight measurement is imprecise. Fourth, the accurate amount of formula or water administered earlier weight loss reaches 10% was not documented. Still this had little effect on weight loss considering minimal corporeality was usually given in a unmarried dose.
Conclusions
An older maternal age, primiparity, and antepartum Caesarean section were constitute to exist independent take a chance factors for excessive weight loss in breastfed full-term newborns in this study. Closer monitoring of these infants is recommended and earlier supplementation with artificial milk may be indicated.
Availability of data and materials
The datasets used and analyzed during the current written report are bachelor from the corresponding writer on reasonable request.
Abbreviations
- BMI:
-
Torso mass alphabetize
- CI:
-
Confidence interval
- NICU:
-
Neonatal intensive care unit
References
-
Flaherman VJ, Schaefer EW, Kuzniewicz MW, Li SX, Walsh EM, Paul IM. Early weight loss nomograms for exclusively breastfed newborns. Pediatrics. 2015;135(one):e16–23.
-
Paul IM, Schaefer EW, Miller JR, Kuzniewicz MW, Li SX, Walsh EM, et al. Weight modify nomograms for the commencement calendar month afterwards birth. Pediatrics. 2016;138(vi):e20162625.
-
Noel-Weiss J, Courant G, Woodend AK. Physiological weight loss in the breastfed neonate: a systematic review. Open Med. 2008;2(4):99–110.
-
Brace AR. Fluid and electrolyte metabolism. In: Polin AR, Fob Due west, Abman Due south, editors. Fetal and neonatal physiology. 3rd ed. Philadelphia: Saunders; 2004. p. 1341–50.
-
McDonald SJ, Middleton P, Dowswell T, Morris PS. Result of timing of umbilical string clamping of term infants on maternal and neonatal outcomes. Cochrane Database Syst Rev. 2013;7:CD004074.
-
Chang RJ, Chou HC, Chang YH, Chen MH, Chen CY, Hsieh WS, et al. Weight loss per centum prediction of subsequent neonatal hyperbilirubinemia in exclusively breastfed neonates. Pediatr Neonatol. 2012;53(1):41–4.
-
Salas AA, Salazar J, Burgoa CV, De-Villegas CA, Quevedo V, Soliz A. Significant weight loss in breastfed term infants readmitted for hyperbilirubinemia. BMC Pediatr. 2009;9:82.
-
Zuppa AA, Sindico P, Antichi Due east, Carducci C, Alighieri G, Cardiello V, et al. Weight loss and jaundice in healthy term newborns in partial and full rooming-in. J Matern Fetal Neonatal Med. 2009;22(9):801–5.
-
Huang A, Tai BC, Wong LY, Lee J, Yong EL. Differential risk for early on breastfeeding jaundice in a multi-ethnic Asian cohort. Ann Acad Med Singap. 2009;38(3):217–24.
-
Yaseen H, Salem G, Darwich M. Clinical presentation of hypernatremic dehydration in exclusively breastfed neonates. Indian J Pediatr. 2004;71(12):1059–62.
-
Pelleboer RA, Bontemps ST, Verkerk PH, Van Dommelen P, Pereira RR, Van Wouwe JP. A nationwide report on infirmary admissions due to dehydration in exclusively breastfed infants in the netherlands: its incidence, clinical characteristics, treatment and outcome. Acta Paediatr. 2009;98(5):807–xi.
-
Shroff R, Hignett R, Pierce C, Marks S, van't Hoff W. Life-threatening hypernatraemic dehydration in breastfed babies. Curvation Dis Kid. 2006;91(12):1025–six.
-
Oddie SJ, Chicken V, Deakin Chiliad, Westman J, Scally A. Severe neonatal hypernatraemia: a population based report. Curvation Dis Child Fetal Neonatal Ed. 2013;98(5):F384–7.
-
Oddie S, Richmond S, Coulthard M. Hypernatraemic dehydration and breast feeding: a population study. Arch Dis Kid. 2001;85(4):318–20.
-
Clarke AJ, Sibert JR. Hypernatraemic dehydration and necrotizing enterocolitis. Postgrad Med J. 1985;61(711):65–vi.
-
Cooper WO, Atherton HD, Kahana M, Kotagal UR. Increased incidence of severe breastfeeding malnutrition and hypernatremia in a metropolitan area. Pediatrics. 1995;96(5 Pt 1):957–60.
-
Kaplan JA, Siegler RW, Schmunk GA. Fatal hypernatremic dehydration in exclusively breastfed newborn infants due to maternal lactation failure. Am J Forensic Med Pathol. 1998;xix(1):xix–22.
-
van Dommelen P, van Wouwe JP, Breuning-Boers JM, van Buuren Due south, Verkerk PH. Reference nautical chart for relative weight change to detect hypernatraemic dehydration. Arch Dis Child. 2007;92(6):490–iv.
-
Caglar MK, Ozer I, Altugan FS. Risk factors for excess weight loss and hypernatremia in exclusively breastfed infants. Braz J Med Biol Res. 2006;39(four):539–44.
-
Johnston M, Landers S, Noble L, Szucs M, Viehmann L. Breastfeeding and the use of human milk. Pediatrics. 2012;129(3):e827–41.
-
Bass JL, Gartley T, Kleinman R. World Health Arrangement baby-friendly infirmary initiative guideline and 2018 implementation guidance. JAMA Pediatr. 2019;173(1):93–4.
-
Becker GE, Remmington T. Early additional food and fluids for healthy breastfed full-term infants. Cochrane Database Syst Rev. 2014;eleven:CD006462.
-
Gartner LM, Morton J, Lawrence RA, Naylor AJ, O'Hare D, Schanler RJ, et al. Breastfeeding and the use of human milk. Pediatrics. 2005;115(2):496–506.
-
Simpson Due east, Goyal NK, Dhepyasuwan N, Flaherman VJ, Chung EK, Von Kohorn I, et al. Prioritizing a inquiry agenda: a Delphi report of the better outcomes through research for newborns (Built-in) network. Hosp Pediatr. 2014;4(4):195–202.
-
Manganaro R, Mamì C, Marrone T, Marseglia L, Gemelli Chiliad. Incidence of aridity and hypernatremia in exclusively breastfed infants. J Pediatr. 2001;139:673–five.
-
Konetzny 1000, Bucher HU, Arlettaz R. Prevention of hypernatraemic dehydration in breastfed newborn infants by daily weighing. Eur J Pediatr. 2009;168:815–eight.
-
Wright CM, Parkinson KN. Postnatal weight loss in term infants: what is normal and do growth charts allow for it? Arch Dis Child Fetal Neonatal Ed. 2004;89:254–vii.
-
Mezzacappa MA, Ferreira BG. Excessive weight loss in exclusively breastfed total-term newborns in a baby-friendly hospital. Rev Paul Pediatr. 2016;34(3):281–6.
-
Fonseca MJ, Severo M, Barros H, Santos Ac. Determinants of weight changes during the first 96 hours of life in full-term newborns. Nativity. 2014;41(2):160–8.
-
Dewey KG, Nommsen-Rivers LA, Heinig MJ, Cohen RJ. Take chances factors for suboptimal infant breastfeeding behavior, delayed onset of lactation, and excess neonatal weight loss. Pediatrics. 2003;112(3 Pt 1):607–19.
-
Davanzo R, Cannioto Z, Ronfani L, Monasta Fifty, Demarini Southward. Breastfeeding and neonatal weight loss in healthy term infants. J Hum Lact. 2013;29(1):45–53.
-
Martens PJ, Romphf L. Factors associated with newborn in-infirmary weight loss: comparisons by feeding method, demographics, and birthing procedures. J Hum Lact. 2007;23(3):233–41.
-
Regnault N, Botton J, Blanc Fifty, Hankard R, Forhan A, Goua 5, et al. Determinants of neonatal weight loss in term-infants: specific association with pre-pregnancy maternal body mass alphabetize and infant feeding mode. Curvation Dis Child Fetal Neonatal Ed. 2011;96(3):F217–22.
-
Implementation guidance. Protecting, promoting and supporting breastfeeding in facilities providing maternity and newborn services—The revised Infant-friendly Hospital Initiative. Geneva: World Health Arrangement; 2018. https://world wide web.who.int/nutrition/publications/infantfeeding/bfhi-implementation/en. Accessed 3 Jan 2020.
-
Baby Friendly Hospital. Nihon Breastfeeding Association. 2019. https://world wide web.bonyu.or.jp/index.asp (In Japanese). Accessed iv Dec 2019.
-
Minkoff H, Chervenak FA. Elective master cesarean delivery. N Engl J Med. 2003;348(x):946–50.
-
Jokic Yard, Guillois B, Cauquelin B, Giroux JD, Bessis JL, Morello R, et al. Fetal distress increases interleukin-6 and interleukin-viii and decreases tumour necrosis factor-alpha cord blood levels in noninfected full-term neonates. BJOG. 2000;107(3):420–5.
-
Shields LE, Goffman D, Caughey AB. Practice bulletin no. 183: postpartum hemorrhage. Obstet Gynecol. 2017;130(iv):e168–86.
-
Grossman X, Chaudhuri JH, Feldman-Wintertime L, Merewood A. Neonatal weight loss at a US infant-friendly hospital. J Acad Nutr Diet. 2012;112(3):410–iii.
-
Marinelli KA, Gill SL, Thulier D. Weighing the facts: a systematic review of expected patterns of weight loss in total-term, breastfed infants. J Hum Lact. 2016;32(1):28–34.
-
Dewey KG, Nommsen-Rivers L, Cohen RJ, Chantry CJ, Peerson JM. Delayed lactogenesis and excess neonatal weight loss are mutual across ethnic and socioeconomic categories of primiparous women in northern California. FASEB J. 2009;23(Suppl ane):344–7.
-
Nishimaki Due south, Okutani T, Tanimura S. Baby friendly hospital data volume 2018. Tokyo: Japan Breast Feeding Association; 2019.
-
Rocha BO, Machado MP, Bastos LL, Barbosa SL, Santos AP, Santos LC, et al. Take chances factors for delayed onset of lactogenesis II among primiparous mothers from a Brazilian baby-friendly infirmary. J Hum Lact. 2020;36(1):146–56.
-
Nommsen-Rivers LA, Chantry CJ, Peerson JM, Cohen RJ, Dewey KG. Delayed onset of lactogenesis amongst commencement-fourth dimension mothers is related to maternal obesity and factors associated with ineffective breastfeeding. Am J Clin Nutr. 2010;92(3):574–84.
-
Scott JA, Binns CW, Oddy WH. Predictors of delayed onset of lactation. Matern Child Nutr. 2007;3(3):186–93.
-
Hurst NM. Recognizing and treating delayed or failed lactogenesis 2. J Midwifery Womens Wellness. 2007;52(6):588–94.
-
Jordan Due south, Emery S, Watkins A, Evans JD, Storey M, Morgan G. Associations of drugs routinely given in labour with breastfeeding at 48 hours: assay of the Cardiff births survey. BJOG. 2009;116(12):1622–9 discussion 1630-2.
-
Zanardo 5, Pigozzo A, Wainer G, Marchesoni D, Gasparoni A, Di Fabio South, et al. Early on lactation failure and formula adoption after elective caesarean delivery: cohort written report. Curvation Dis Child Fetal Neonatal Ed. 2013;98(1):F37–41.
-
Heasman L, Spencer JA, Symonds ME. Plasma prolactin concentrations after caesarean section or vaginal delivery. Arch Dis Kid Fetal Neonatal Ed. 1997;77(3):F237–8.
-
Uvnäs Moberg G, Prime DK. Oxytocin effects in mothers and infants during breastfeeding. Infant. 2013;9(6):201–6.
-
Omar SA, DeCristofaro JD, Agarwal BI, La Gamma EF. Effects of prenatal steroids on water and sodium homeostasis in extremely low nascency weight neonates. Pediatrics. 1999;104(three Pt 1):482–eight.
-
Feeney JG. Water intoxication and oxytocin. Br Med J (Clin Res Ed). 1982;285(6337):243.
-
Noel-Weiss J, Woodend AK, Peterson WE, Gibb Due west, Groll DL. An observational written report of associations among maternal fluids during parturition, neonatal output, and breastfed newborn weight loss. Int Breastfeed J. 2011;six:9.
Acknowledgements
We sincerely thank Dr. Ichiro Yasuhi, Dr. Hiroshi Yamashita, and Dr. Sachie Suga (Department of Obstetrics and Gynecology, National Infirmary Organization Nagasaki Medical Middle, Nagasaki, Japan) for helpful discussions and valuable communication regarding the statistical analyses.
Funding
This enquiry did non receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Affiliations
Contributions
YM conceived the report idea, collected information, performed the information analysis, and wrote the manuscript. HS, MA, and ST reviewed and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This report was approved by the Enquiry Ideals Committee of the National Hospital Organisation Nagasaki Medical under protocol number 2019079, canonical on October x, 2019, with opt-out consent to obtain patient data from the medical records.
Consent for publication
Non applicative.
Competing interests
The authors declare no conflicts of interest in association with the nowadays study.
Boosted information
Publisher'due south Notation
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long every bit you give appropriate credit to the original author(s) and the source, provide a link to the Artistic Commons licence, and betoken if changes were made. The images or other third party material in this commodity are included in the article's Artistic Eatables licence, unless indicated otherwise in a credit line to the material. If fabric is not included in the article's Artistic Eatables licence and your intended use is not permitted past statutory regulation or exceeds the permitted use, you lot will demand to obtain permission directly from the copyright holder. To view a re-create of this licence, visit http://creativecommons.org/licenses/past/four.0/. The Artistic Eatables Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zilch/1.0/) applies to the data made bachelor in this article, unless otherwise stated in a credit line to the data.
Reprints and Permissions
Most this article
Cite this article
Miyoshi, Y., Suenaga, H., Aoki, M. et al. Determinants of excessive weight loss in breastfed total-term newborns at a baby-friendly hospital: a retrospective cohort report. Int Breastfeed J 15, nineteen (2020). https://doi.org/10.1186/s13006-020-00263-two
-
Received:
-
Accepted:
-
Published:
-
DOI : https://doi.org/x.1186/s13006-020-00263-2
Keywords
- Newborn
- Breastfeeding
- Nascence weight
- Weight loss
- Caesarean department
Source: https://internationalbreastfeedingjournal.biomedcentral.com/articles/10.1186/s13006-020-00263-2
0 Response to "Ps Ot Normal for Babies to Lose Weight Right After Birth"
Post a Comment